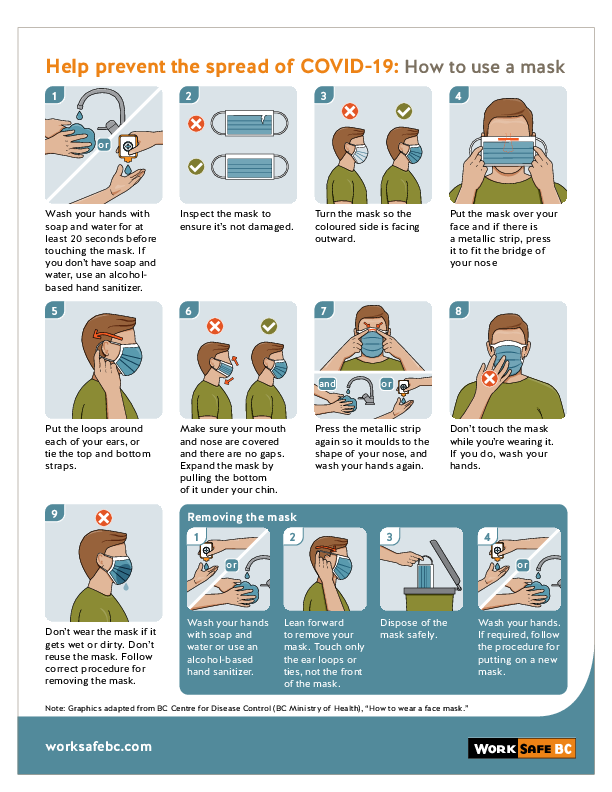
Personal Protective Equipment
iwh.on.ca
Study conducted at the start of the COVID-19 emergency finds workers who felt safe at ...
their physical worksites had better mental health than workers who felt workplace COVID-19 safety practices were inadequate
Adequate COVID-19 protections such as personal protective equipment (PPE) and workplace infection control protocols (ICP) are linked to the mental health of workers. This is according to a new Institute for Work & Health (IWH) study of Canadian workers conducted in the spring of 2020—a second study to find such link between workplace protection and workers’ mental health in the first weeks of the emergency.
The study, conducted jointly with the Occupational Health Clinics for Ontario Workers (OHCOW), found symptoms of anxiety and depression were highest among people who continued to go to work during the lockdown but felt none of their needed PPE and ICP protections were in place. In contrast, anxiety and depression symptoms were least prevalent among people who physically went to work but felt all the needed measures and PPE were available.
Notably, people who felt fully protected at their worksites had similar or even slightly better mental health compared to people who worked from home. Likewise, people who felt entirely unprotected at work had even poorer mental health than people who had lost their jobs since the start of the pandemic.
The study, accepted for publication in the Annals of Work Exposures and Health, was based on a survey conducted by IWH and Occupational Health Clinics for Ontario Workers (OHCOW) in the spring of 2020. The analysis compared anxiety and depression symptoms across three groups of workers. These were: people who worked remotely (42 per cent of the sample); people who were at work at their workplace (51 per cent of the sample) and people who had lost their job since the onset of the pandemic (seven per cent).
The findings reinforce the importance of personal protective equipment (PPE) and workplace infection control protocols (ICP)—not only to prevent COVID-19 transmission but also to safeguard workers’ mental health, says IWH Senior Scientist Dr. Peter Smith and lead author of the journal article.
This pandemic has taken a toll on people’s mental health—whether due to prolonged isolation or financial distress or fears of infection, says Smith. One way that workplaces can minimize the risks of anxiety and depression for workers is to offer those who have to come to work the equipment and protocols they need to stay safe from COVID. That’s a message that is just as important now, as case numbers are once again on the rise, as was the case in the spring.
Online surveys shared by labour networks
The survey at the heart of this study was one of two sent out by OHCOW and a network of labour organizations from April to June 2020. Both were focused on on understanding the experiences of different groups of workers during the early stage of the COVID-19 pandemic. The first survey, designed for health-care workers, drew almost 6,000 participants; findings from that survey were published in September in the Canadian Journal of Psychiatry (doi:10.1177/0706743720961729).
The second survey, designed for workers outside the health-care sector, was completed by more than 3,500 participants. They were asked four questions from two widely used anxiety and depression clinical screening tools. From the Generalized Anxiety Disorder screener, they were asked how often they felt nervous, anxious, on edge or not able to stop worrying. From the Patient Health Questionnaire-2 screener, they were asked how often they felt little interest or pleasure in doing things or felt down, depressed or hopeless. In the analysis, the research team focused on the share of respondents whose scores were above the accepted threshold for clinical screening of anxiety and depression.
Respondents who worked on-site were asked to gauge their need for 10 different types of PPE, which included gloves, eye protection, face shields, gowns or coveralls, surgical masks, N95 masks and respirators. They were also asked about 14 different IPCs, including increased ventilation, installation of plexiglass or other barriers, isolation of people, physical distancing from customers, physical distancing from co-workers and frequent cleaning. Participants were also asked about the adequacy of the PPE and IPC they said they needed.
The study found that the group working on-site with all needed protection had similar, if not slightly better, mental health levels as those working from home. Anxiety and depression symptoms were reported by 35 per cent and 27 per cent of remote workers respectively; they were reported by 30 to 34 per cent and 23 to 25 per cent of on-site workers with all their needs met.
More noteworthy were the anxiety and depression levels among people who said they had no protection at their physical worksites. With 52 per cent and 46 per cent reporting anxiety and depressive symptoms respectively, this group even had significantly poorer mental health than people who lost their jobs. In this latter group, anxiety and depression levels were experienced by 44 per cent and 36 per cent of respondents, respectively.
It’s worth noting that we saw a significant amount of fear, stress, concern, depression and anxiety among workers, says Smith, adding that the study design does not allow the team to pinpoint whether people are stressed out over their financial situations, their children’s schooling or their safety at work. As more and more Canadians return to the workplace, this study suggests that the adequacy and effectiveness of COVID-19 infection procedures have important implications, not only for reducing COVID-19 rates, but for the mental health of the workforce, he adds.
Stay up to date and sign up for one of our newsletters for more topics on Health and Wellness, Commercial Vehicle Safety and more!